Extensor Hallucis Longus Muscle
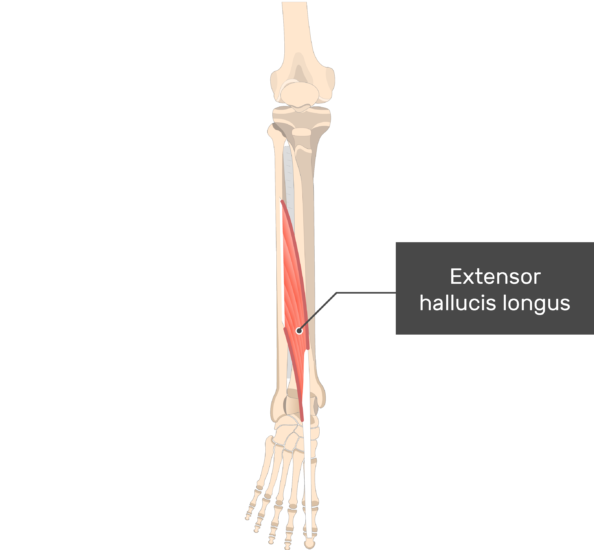
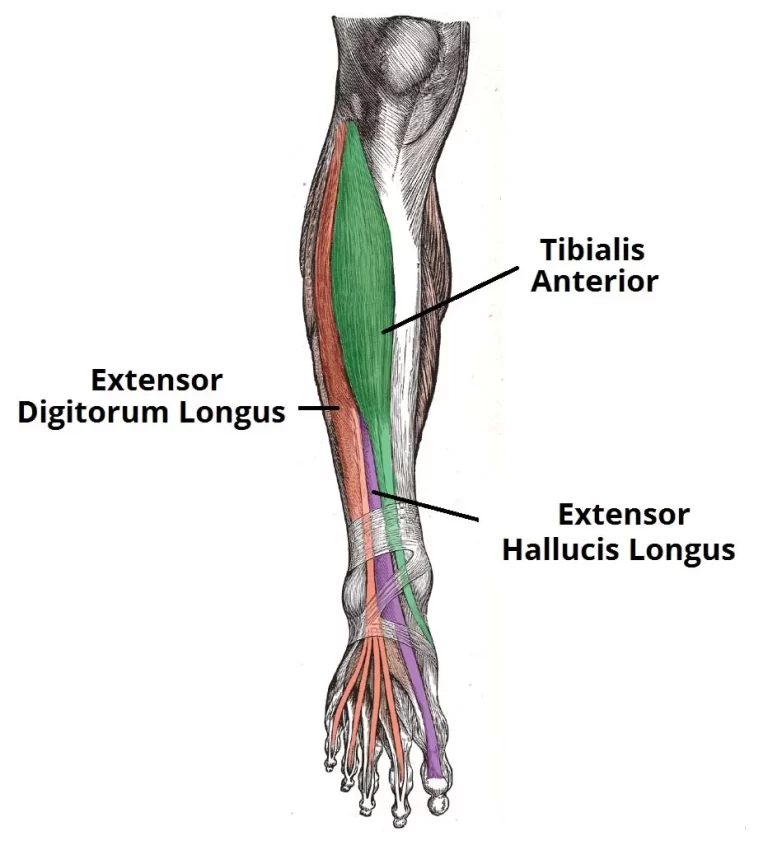
Extensor Hallucis Longus Muscle Anatomy The extensor hallucis longus is a skeletal muscle located in the anterior compartment of the leg. It plays a crucial role in the movement of the foot and toes, specifically in the extension of the big toe. Extensor hallucis longus muscle is a thin muscle that extends from the middle…